Tag: Moore
Control Your Breathing
Check out our newest video on some simple strategies to help control your breathing and it’s effects on the body!
What is Women’s Health/Pelvic Floor Physical Therapy?
Today’s blog post is from our Women’s Health Specialist and OSSPT physical therapist, Jenna Jarvis. We hope you enjoy and share with your friends.
When I started physical therapy school, I suspected I would likely work in an orthopedic and sports setting; however, I never suspected I would become a Women’s Health Specialist and treat pelvic floor dysfunctions. In fact, prior to physical therapy school, I did not even know women’s health or pelvic floor therapy existed. People often ask me what led me down this path and why I chose this specialty. In reality, I didn’t choose to become a Women’s Health Specialist as much as it chose me.
Beginning in my first year of physical therapy school, I started developing a constant, aching pain in the back of my right hip and thigh when sitting for long periods of time while studying or riding in the car while commuting to school. Not long after, I began experiencing pain with running, my main outlet from the stress of school. After a few weeks of continued pain, with no help from any of the exercises I “Googled” online and knew from PT school already, I decided to schedule an appointment with a physical therapist for further evaluation. After a few weeks of treatment, I still noticed only a minimal difference in my symptoms and became quite frustrated with my situation. I continued consulting with other physical therapists and an orthopedic surgeon, but never found any answers or treatment that relieved my pain. I started to feel a little crazy, and question whether it was all in my head. My pain was so intense, I could hardly sit in the car without a cushion and I had to stand in the back of the classroom during lectures. Most frustratingly, I could no longer run due to the pain being so severe.
Nine months of continued, unrelenting pain later, we had a guest lecturer present about women’s health physical therapy. As I stood in the back of the room (remember the pain was too intense to sit), she presented a case study of a 20 year old female who had pain with running and sitting. As she continued discussing the case, all the symptoms matched mine entirely. I knew I needed to explore this treatment more. After class, I talked with the Women’s Health Specialist and she confirmed that, in fact, a lot of my symptoms were common with pelvic floor dysfunctions and that she felt confident she could help me. To this day, I can still not explain the amount of relief I felt to know that my symptoms, not only made sense, but that a solution was also available as well. Within the first few weeks of treatment, I already noticed a reduction in pain, returned to some light running, and I could finally sit in class again. Within a few months of treatment, I was at least 95% better and ran my first marathon, qualifying for the Boston Marathon. I finally had my normal life back!
Following my personal experience and success with pelvic floor therapy, I knew I wanted to offer these same services to my future patients. Knowing that these advanced women’s health treatments were not taught in PT school, I found and attended some of the most advanced and respected pelvic floor and women’s health courses and completed a long term clinical rotation with one of the premiere women’s health specialists in the country treatments women with pelvic floor dysfunctions on a daily basis. Additionally, I am constantly learning more about this specialty every day. In my experiences, I am always astonished with how many of patients have lived through years of pelvic and low back pain with no answers before they discovered pelvic floor therapy. Pelvic floor physical therapy is truly my passion and my professional mission is to educate the medical field and the public about pelvic floor therapy and its benefits.
What is Pelvic Therapy/Women’s Health Physical Therapy?
Pelvic floor physical therapy is a common term for a thorough examination, assessment, and treatment of the thoracic, lumbar, and sacral spine, pelvis, and lower extremities and various related physiological systems that could be causing pain or dysfunction. Pelvic floor therapy is also known as women’s health physical therapy, pelvic floor physical therapy, pelvic rehab, or urogynecological physical therapy. In addition to the pelvic realm, women’s health therapy can also be beneficial for women following breast cancer and radiation treatment to address pain, decreased upper extremity mobility, and other dysfunction related to treatment of cancer.
Who can benefit from Pelvic Therapy/Women’s Health Therapy?
Pelvic and women’s health therapy can be beneficial for patients experiencing the following:
- Urinary incontinence
- Pelvic pain
- Pregnancy and post-partum
- Bowel incontinence
- Constipation
- Fibromyalgia
- Pelvic organ prolapse
- Scarring from abdominal surgeries
- Post-partum- Cesarean section or vaginal delivery
- Diastasis recti (separation of the abdominal muscles)
What are common signs and symptoms of a Pelvic Floor Dysfunction?
- Urinary leakage with coughing, sneezing, or laughing (although urinary incontinence is common, it is not normal in any situation)
- The urge to urinate frequently or a sudden, uncontrollable urge to urinate immediately
- Waking up multiple times throughout the night to urinate
- Pelvic, lumbar, thoracic, or lower extremity pain
- Pain with sitting
- Pain with sexual intercourse
- Chronic urinary tract infections
Where does Pelvic Floor Dysfunction Pain Refer to?

What can I expect with pelvic floor therapy?
In your first visit, you can expect a thorough examination of your past medical history, eating, drinking, voiding, and sexual habits and how they may relate to your pain or dysfunction. In addition, an examination of the thoracic and lumbar spine, pelvic, and lower extremities will be done to assess any orthopedic dysfunction that could be contributing. Finally, an examination of strength and control of the surrounding musculature will be assessed, which will include an external and possibly an internal examination. Patient comfort and safety is always my top priority. I understand that every patient will have differing levels of comfort and we can always modify the examination and treatment to the patient’s preference.
What treatments are used for physical therapy?
Treatment for pelvic floor therapy may include, but is not limited to the following:
- Pelvic floor, core, and lower extremity exercises and re-training
- Soft tissue mobilization
- Joint and spinal mobilization and manipulation
- Creating a bladder diary to track progress
- Diet education
- Behavioral techniques and education
- Postural and functional retraining
Kegel exercises are specific exercises that focus on strengthening the pelvic floor. Although these exercises can be beneficial in the right situation, Kegel exercises do not fix all pelvic floor dysfunctions. In fact, often times Kegel exercises magnify a patient’s symptoms. Pelvic floor dysfunctions are not caused purely by weakness; they are due to an inability to properly engage the pelvic floor musculature, which can be either over-active or under-active musculature. This is one of the biggest reasons why a patient cannot simply “Google” their problem and why they need to be individually evaluated by a specialist to determine the true cause of their pelvic floor dysfunction and to create an individualized plan to properly retrain the pelvic floor musculature.
When a patient is experiencing a significant pelvic floor dysfunction it can be debilitating and life altering. To make matters worse, resources to address these issues are often limited; patients are often initially misdiagnosed and improperly treated. If you are someone who has been suffering from a possible pelvic floor dysfunction, please do not give up. I have been in your shoes and I can help. If you have any additional questions or would like to schedule an evaluation, please call us at (405) 735-8777.
Latissimus Tears: The Newest Injury for Throwing Athletes (Part II)
Just when you thought rehabbing pitchers was hard enough, a new injury has emerged in the throwing population
If you haven’t read Part I of our series, please check it out now. In part I we discussed anatomy, how the lats are in involved with pitching, reasons for the increase in lat injury frequency, and a brief surgical review.
For Part II, we are discussing common compensations we see in the “lat dominant” population and demonstrate a few examples of our favorite functional exercises to retrain this dominance with video demonstration by OSSPT patient and San Francisco Giants prospect, Caleb Simpson.
As previously mentioned, the lats have multiple attachment sites, spanning across several joints in the body, including the thoracic and lumbar spine, pelvis, ribs, scapula, and humerus. Because of all these various attachment sites, the lats have a major influence on posture, breathing, pelvic control, scapular mobility, and glenohumeral positioning. When the lats are working properly, they are crucial in power development with throwing; however, when the lats become too dominant, they are at risk of injury.
Although we are big believers of implementing deadlifting, horizontal/vertical pulling, and carrying into an athletes plan of care, we need to make sure the lats do not become the dominant muscle with all lifts for the throwing athlete. When presented with a task that is too demanding for the throwing athlete, he/she will revert to over-utilizing the dominant muscles. Our job as physical therapists is to, first identify these compensations, then educate and correct the athlete of proper movement patterning. We must prescribe the athlete with exercises that are challenging, but also achievable.
To assist with better identifying when the lats may have become too dominant, we have listed some common compensation patterns to look for.
Common “Lat Dominant” Compensations
1. Excessive lumbar extension/anterior pelvic tilt: with attachments  to the thoracolumbar fascia, spine, and pelvis, overly dominant lats will often lead to excessive lumbar extension and an anteriorly pelvic tilted position. Overly-dominant muscles often lead to shortened muscles so we need to incorporate exercises that force the lats to work in an eccentric, lengthened position while maintaining a neutral spine.
to the thoracolumbar fascia, spine, and pelvis, overly dominant lats will often lead to excessive lumbar extension and an anteriorly pelvic tilted position. Overly-dominant muscles often lead to shortened muscles so we need to incorporate exercises that force the lats to work in an eccentric, lengthened position while maintaining a neutral spine.
2. Faulty breathing mechanics: most of our patients, particularly our athletes, have poor diaphragmatic breathing and often over recruit the accessory respiratory muscles, including the lats. Many of the accessory respiratory muscles further pull the body into a lumbar extended, anteriorly pelvic tilted position. At rest, we breathe approx. 15,000-20,000x/day. If we are constantly breathing improperly, the lats are living in faulty, shortened positions. We spend a lot of time teaching proper diaphragmatic breathing to our throwing athletes and incorporate diaphragmatic breathing into our exercises when possible.
3. Rib flaring: the first two compensations we discussed will often lead to rib flaring, so if we correct the excessive lumbar lordosis/anterior pelvic tilt and faulty breathing mechanics, the rib flare may resolve; however, a  rib flare can also develop due to weakness of the anterior core. With our throwing athletes, we must incorporate anterior core control exercises while in an overhead position. This will ensure our pitchers can successfully control the rib cage, which is vital to ensure proper scapular position as well.
rib flare can also develop due to weakness of the anterior core. With our throwing athletes, we must incorporate anterior core control exercises while in an overhead position. This will ensure our pitchers can successfully control the rib cage, which is vital to ensure proper scapular position as well.
4. Shoulders falling into IR and/or adducted positions: the most common technique used to identify this compensation pattern is the prone horizontal abduction exercise. Instead of the shoulder remaining at 90 deg. during the arm raise, the overly dominant lat will pull the arm down toward the hip (as you can see in the picture below). In early stages of rehab, teaching and performing this exercise correctly can be an appropriate intervention to reduce the lat dominance and improve mid trap and rhomboid activation with this movement.
 5. Insufficient scapular elevation/upward rotation: due to the lats attachment to the inferior aspect of the scapula, “dominant lats” can lead to depressed scapula, or at the minimum, dominant lats can prevent proper scapular elevation/upward rotation with overhead movements. For the throwing athlete, a lack of proper scapular control and movement will lead to impaired glenohumeral joint congruency and contribute to rotator cuff/labral pathology.
5. Insufficient scapular elevation/upward rotation: due to the lats attachment to the inferior aspect of the scapula, “dominant lats” can lead to depressed scapula, or at the minimum, dominant lats can prevent proper scapular elevation/upward rotation with overhead movements. For the throwing athlete, a lack of proper scapular control and movement will lead to impaired glenohumeral joint congruency and contribute to rotator cuff/labral pathology.
Exercise Examples
1.Plank –> Downward Dog: an excellent upper extremity closed chain movement that promotes proper scapular upward rotation and requires anterior core control, while putting the lat in a lengthened position. We cue the athlete to drive thru the palms, maintain a neutral spine, and bring the hips to the sky. We will use this exercise as a primer before introducing higher level overhead movements.
2. MedBall Lat Pullovers: this exercise forces the athlete to maintain a neutral spine, not allow rib flaring while controlling the medball overhead, and teaches proper eccentric lat control. We will often incorporate diaphragmatic breathing techniques while in the overhead position as well. Just like our previous exercise, this can be another primer movement.
3. Wall Angels: this exercise is an excellent choice for the general population to address common postural dysfunctions including excessive lumbar lordosis, anterior pelvic tilt, increased thoracic kyphosis, rounded shoulders, and forward head positioning. To perform correctly, the athlete cannot allow rib flaring either.
4. Half Kneeling S.A. 90-90 Row-ER-Press: as we progress through our exercise examples, we are gradually increasing loads as well. With this exercise, we continue to demand proper core control, emphasized by adding an unstable surface via the Dynadisc for the R knee. This exercise also demands proper posterior rotator cuff activation as we cue the athlete to drive his fist straight to the sky during the press movement. To better replicate the pitching demands and mimic a glove side pulling that many pitching coaches instruct with an isometric glove side row.
5. Unilateral Overhead KB Marches: this exercise is a great stability based exercise in multiple planes of movement, particularly when we add the band resistance as well. The big thing to watch for is excessive lumbar extension, rib flare, pelvic drop, or the athlete not keeping the KB shoulder in full flexion with slight shoulder ER. We cue them to drive the KB to the sky w/o allowing the shoulder to shrug. As we can see in the video below, Caleb is having some difficulty with maintaining extended elbow position and he is allowing the shoulder to rotate internally.
6. Tall Kneeling Halos: our last exercise may look easy from the surface, but halos will reveal compensations really quickly. This exercise demands excellent core stability and a combination of excellent shoulder stability and mobility.
The lats are important muscles for the throwing athlete and it’s vital that we identify and correct common movement dysfunctions and implement appropriate exercises to re-train these faulty movement patterns.
I hope you enjoyed our 2 part blog post. I wanted to provide a quick shout out to Mike Reinold and Eric Cressey. I was introduced to these two guys eight years ago while working with the Atlanta Braves and I have attempted to read everything they have produced since that time and they are two of the biggest influences in my professional career. Both guys put out great material on a daily basis and so much of how I treat our baseball players is either directly or indirectly influenced by them, including this blog post. I want to say a big thank you to Mike and Eric for how much they have helped, not only me, but the medical and performance profession as a whole.
Latissimus Tears: The Newest Injury for Throwing Athletes (Part I)
Just when you thought rehabbing pitchers was hard enough, a new injury has emerged in the throwing population
With Spring Training underway, baseball is officially back! As a fan, I am more than excited. As a medical professional and a PT who spends a lot of time treating the baseball population, I know my schedule is about to ramp up. As Posner, et al (2011) found, April is the month with the highest injury rates for MLB players, with pitchers having a 34% higher injury than position players. One of the injuries we are seeing more often than in years past in our professional pitchers are latissimus injuries. For a lot of reasons, we will discuss below, it seems that latissimus injuries are being diagnosed more frequently than they were in decades past. It was not until 2010 that the first lat repair surgery was performed on a professional baseball player, when Jake Peavy went under the knife. Since then, many of the game’s biggest stars, including Stephen Strasburg, Fernando Rodriguez, Clayton Kershaw, Noah Syndergaard, and Cardinals top prospect Alex Reyes have sustained lat injuries. In a systematic review of 30 professional baseball pitchers, Mehdi, Frangiamore, & Schickendantz (2016) found that the average time required to return to pitching was 99.8 days for the non-operative group and 140 days for the surgically treated group. As you can see, once you sustain a lat injury, the recovery is slow.
Because so few PT’s in the traditional clinic setting treat professional athletes on a regular basis, we created a massive two part blog for our audience to serve as an additional resource to develop a better understanding of the injury and implications for pitchers. We hope you will enjoy!
In Part I, we will review latissimus anatomy and it’s involvement with pitching, theories for the increase in lat injuries for professional pitchers, and a brief review of the surgery.
In Part II, we will discuss common compensations for “lat dominant” athletes and demonstrate a few of our favorite functional exercises that specifically focus on addressing the common compensation patterns.
Anatomy
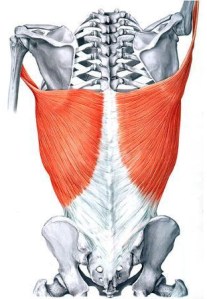
The latissimus dorsi is the largest and most powerful muscle in our backs, originating from the T7-L5 vertebrae (basically our bra straps to our belt line), the thoracolumbar fascia, iliac crest, the bottom 3-4 ribs, and the inferior aspect of our scapula. The lats then insert on the intertubercular groove of the humerus. THAT’S A LOT OF ATTACHMENTS, LEADING TO A LOT OF MOVEMENT INFLUENCES. To make matters more complicated, the lats have a lot of variability in respect to its specific attachment sites.
The general functions of the lats include extension, adduction, cross body adduction, and internal rotation of the shoulder. For many recreational lifters, the lats become the dominant muscle with all vertical and horizontal pulling movements such as rows, pull ups, and pull downs.
How are the Lats involved with Throwing?
For baseball pitchers, the lats are one of the most important muscles in developing arm speed, and therefore, increasing throwing velocity. As Eric Cressey (2016) has previously stated, the lat “connects the lower body to the upper body to allow for force transfer that ultimately leads to arm speed and ball velocity”. The lats have several very specific and important functions in the pitching motion, including the following:

- Initially, the lats work eccentrically during the cocking/lay back phase to control the shoulder external rotation occurring.
- When a muscle is working eccentrically, it is being lengthened under load. When a muscle is working concentrically, it is being shortened under load. For example, when you do a biceps curl, the curl portion of the movement is a concentric movement (shortening of biceps). As we slowly lower the weight, we are still using the biceps muscle eccentrically (lengthening of the biceps).
- Next the lats transition from eccentrically lengthening (storing elastic potential energy) during the cocking/lay back phase to concentrically shortening (utilizing that stored energy to generate high arm speeds) during the arm acceleration phase.
- Finally the lats continue working concentrically as the arm accelerates during throwing to release, acting as one of the major force generators during this phase. According to Fleisig, Andrews, Dillman, & Escamilla (1995), the throwing arm accelerates at over 7000 degrees per second, which is the fastest recorded human motion in sports (3).
The further the lay back phase, the mo re the elastic potential energy created by the lats, thereby providing more opportunities for increased velocity. If you look at the picture below of Billy Wagner, one of the hardest throwing pitchers in the history of the game, you can appreciate the considerable amount of layback in his throwing shoulder, and it quickly makes sense how he became of the games hardest throwers. He generated vast amounts of elastic potential energy via the lats.
re the elastic potential energy created by the lats, thereby providing more opportunities for increased velocity. If you look at the picture below of Billy Wagner, one of the hardest throwing pitchers in the history of the game, you can appreciate the considerable amount of layback in his throwing shoulder, and it quickly makes sense how he became of the games hardest throwers. He generated vast amounts of elastic potential energy via the lats.
If the idea of elastic potential energy is still confusing, then check out this short video below which provides additional information.
What Does all that Energy Talk Mean Injury Wise?
Muscles and tendons, throughout the body, are most vulnerable to injury during the eccentric phase of movement (being lengthened). When you add large loads to the eccentric phase, as seen when throwing a baseball, and then ask the muscle-tendon complex to transition from being maximally lengthened to concentrically contracted at high speeds , we are asking for trouble. As you can see, the demands on the lats are very high during the throwing phase.
To provide a better visualization of what happens when you overload a muscle/tendon during the eccentric phase, check out this video below (beware of language). At the 30 second mark, you will see a lady (wearing the ironic “Today is the Day” shirt) take a quick step back with her left leg, leading to an eccentric stretch to the Achilles, followed by an attempt to quickly concentrically contract and shorten her Achilles. Unfortunately for her, she overloads the tissue, rupturing her Achilles (if you don’t mind the language, you can literally hear the pop happen).
Why the Increase in Lat Injuries?
Clearly, pitching places a lot of demands and stresses on the body, particularly the lats, but the question remains, why such sudden increases in lat specific injury risk? The answer appears to be multi-factorial. Below, I have listed some of the probable causes.
-
- Pitchers are throwing harder: From 2008-2017 the average 4-seam fastball increased from 90.9 mph to 93.2 mph. Additionally, in 2008, there were only 196 pitches thrown 100+ mph in the league for the entire season. In 2017, there were over 1,000 pitches thrown 100+ mph for the league (Clair, 2018). As throwing velocity increases, so do the stresses placed on the entire body as whole; furthermore, Gowan, et al (1987) showed that professional pitchers (harder throwers) have a much higher lat recruitment during the arm acceleration phase than amateurs. Simply put, velocity is rising, and as velocity rises, so do the stresses placed on the lats.
- Pitching Year Around: Year around throwing is the root of all evil. At OSSPT, we tell our pitchers that the risks of year around throwing are analogous to the risks of smoking. Similar to how smoking is the top risk factor for many health conditions, year around throwing is the top risk factor for almost all throwing injuries. As amateur pitchers constantly jump from school ball to travel ball, and then indoor lessons, they never allow their body to take a break, resulting in excessive cumulative stresses placed on the lats, and body as a whole. Also, we know that as we throw throughout the year, our body undergoes some specific changes which further increase lat injury risk. For example, we know that throughout the season, pitchers have a significant decrease in shoulder internal rotation, total motion, and elbow extension (Reinold, et al, 2008). Also, Zeppieri et al (2015) showed that collegiate pitchers lose hip ROM and strength throughout the throwing season. Besides simply reducing the amount of cumulative stresses placed on the body, we also must take time off from throwing to receive adequate rehab to regain strength and motion losses prior to the next season.
- The American Sports Medicine Institute has released throwing guidelines and recommends no overhead throwing of any kind for a minimum of 2-3 months per year(http://www.asmi.org)
- Weighted Ball Programs: Because pitchers and performance coaches are constantly searching for ways to increase velocities, weighted balls have become the newest trend in baseball. Based on the literature from Reinold et al. (2018), a 6 week weighted ball throwing program led to a 3.3% increase in throwing velocity. A velocity jump like that could be the difference between AA ball or the majors. All good news right? Not quite, Reinold et al. (2018) showed that the weighted ball group had a 4.3° degrees increase in external rotation, meaning more lay back, which may explain the velocity jump, but it also means increased eccentric loading for the lats as well. Not surprisingly, in the study, the weighted ball group also had a 24% injury rate, while the control group had no injuries during the 6 weeks period. Although the usage of weighted balls appears to have some performance benefits, we are still uncertain of how to safely implement these throwing programs in regards to how often, how heavy should the weighted balls be, what ages are most appropriate, etc. Because of all the uncertainties surrounding weighted balls, we strongly recommend that you proceed cautiously when attempting a weighted ball program.
- Lat Dominance/Faulty Training: We will discuss this in much more detail in Part II, along with providing some of the exercises we utilize to retrain our lat dominant throwing athletes.
Surgery
While most lat injuries are Grade I or II strains (partial tears), occasionally a throwing athlete will sustain a tear large enough that requires surgical intervention. Dr. Anthony Romeo performed the first lat repair surgery on a MLB player and has become the pioneer of the lat repair surgery. According to Dr. Romeo’s website,
“The latissimus dorsi repair is done by making an incision in the back of arm, near the armpit. The ruptured tendon is then located, and sutures are placed in the end of the torn tendon. Those sutures are then used to pull the tendon back up to the arm bone where the tendon ruptured. Small metallic anchors, called buttons, are then used to fix the tendon to the bone.” (https://www.romeoorthopaedics.com/surgeries/latissimus-dorsi-repair).
In the picture below, you can see OSSPT patient and San Francisco Giants prospect Caleb Simpson’s incision following his lat repair surgery.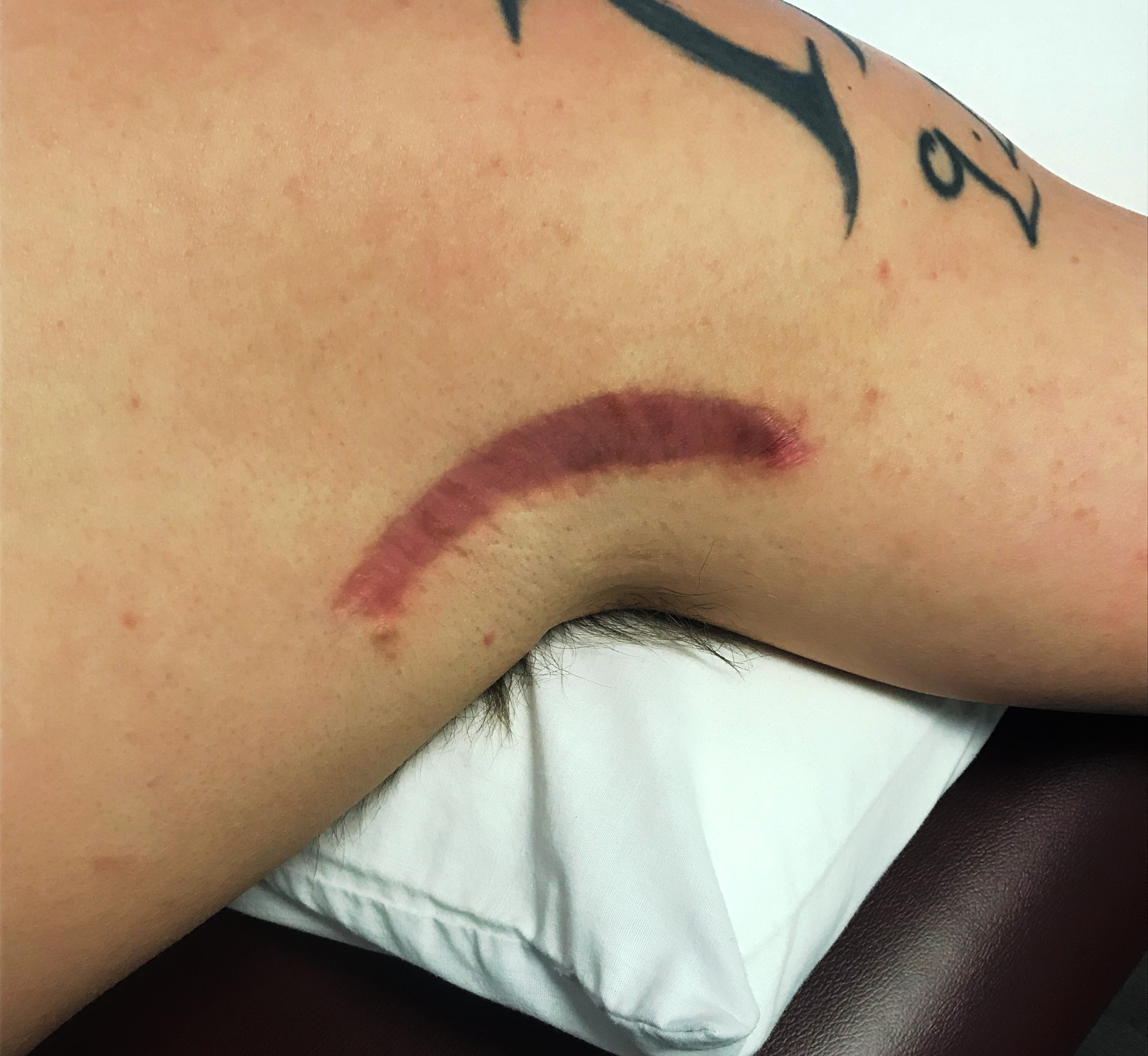
To check out Part II, click here.
References
Clair, M. (2018, August 29). Are pitchers really throwing harder than ever? Retrieved from https://www.mlb.com/cut4/are-pitchers-really-throwing-harder-than-ever/c-292153594
Cressey, E. (2016, May 4). Pitching injuries: should lat strains even be happening? Retrieved from https://ericcressey.com/pitching-injuries-lat-strains
Cressey, E. (2018, July 9). 5 reasons for the increase in lat strains in baseball pitchers. Retrieved from https://ericcressey.com/5-reasons-lat-strains-baseball-pitchers
Fleisig, G. S., Andrews, J. R., Dillman, C. J., & Escamilla, R. F. (1995). Kinetics of baseball pitching with implications about injury mechanisms. The American Journal of Sports Medicine, 23(2), 233–239. https://doi.org/10.1177/036354659502300218
Gowan, I. D., Jobe, F. W., Tibone, J. E., Perry, J., & Moynes D. R. (1987). A Comparative Electromyographic Analysis of the Shoulder During Pitching. Professionals versus Amateur Pitchers. The American Journal of Sports Medicine, 15(6), 586-590.
Mehdi, S.K., Frangiamore, S.J., & Schickendantz, M.S. (2016). Latissimus dorsi and teres major injuries in major league baseball pitchers: a systematic review. American journal of orthopedics, 45(3), 163-167 .
Posner, M., Cameron, K., Wolf, J., Belmont, P., & Owens, B. (2011). Epidemiology of major league baseball injuries. The American Journal of Sports Medicine, 39(8), 1676-1680.
Reinold, M.M., Macrina, L. C., Fleisig, G. S., Aune, K., & Andrews, J. R. (2018). Effect of a 6-week weighted baseball throwing program on pitch velocity, pitching arm biomechanics, passive range of motion, and injury rates. Sports Health, 10(4), 327-333.
Reinold, M.M., Wilk, K.E., Macrina, L.C., Sheheane, C., Dun, S., Fleisig, G.S., Crenshaw, K., & Andrews, J.R. (2008). Changes in shoulder elbow passive range of motion after pitching in professional baseball players. American Journal of Sports Medicine, 36(3), 523-527.
Zeppieri, G., Lentz, T., Moser, M., & Farmer, K. (2015). Changes in hip range of motion and strength in collegiate baseball pitchers over the course of a competitive season: A pilot study. International Journal of Sports Physical Therapy. 10, 505-513.
https://www.physio-pedia.com/Throwing_Biomechanics (picture)
We Must Build a Foundation Before We Can Build Walls
A few nights ago, I couldn’t sleep and ended up watching a show about the construction of the Burj Khalifa, the tallest building in the world. In the show, they mentioned that the design used approx. 50% the amount of steel used in the construction of the Empire State Building, which is half the height of the Burj Khalifa. That fact initially surprised me, before realizing it was a simply matter of improved design efficiency and building a better foundation which could tolerate higher loads. That concept brought me back to one of our principal philosophies we apply at OSSPT, which is to ensure we build a better foundation of movement quality, before we ever increase movement quantity. The foundation of physical therapy should be about correcting faulty movement patterns.
“Tarzan, to me, is the epitome of fitness. The guy is strong, agile and quick. He can run, jump, climb and swing through trees. If we take a person who moves well and put them on a Crossfit type of training program, we turn them into Tarzan. If we take that same program and give it to the majority of people in society who move poorly, we turn them into a patient.”
– Gray Cook
Faulty movement patterns are the underlying reason behind ALL chronic conditions and many acute injuries. Without fixing the foundation, we are fighting a losing battle and eventually the walls will come crashing down, whether that be a recurrence of previous injury, worsening of current symptoms, or simply developing a new injury complaint. The number one risk for musculoskeletal injury is a previous injury, clearly indicating that something we are doing in the rehabilitation process is wrong and insufficient.
Ever wonder why your hip or knee become arthritic on one side and not the other? Ever wonder why your neck or low back are not getting better with years of adjustments, massages, etc? Ever wonder how you developed bone spurs in your your foot, heel, hip, shoulder, etc? The most likely answer is that you moved incorrectly, year after year, until finally, you developed structural changes, and then pain. As Gray Cook asks, are you moving poorly because you are in pain? Or are you in pain because you are moving poorly? We know that structural changes begin before we start experiencing pain, and we know that structural changes happen when we move improperly; therefore, we know that faulty movements lead to pain overtime. Here’s the great news… we can change how we move and if we change how we move we have an excellent opportunity to eliminate the pain cycle once and for all. 
Try this quick test… perform a squat just like the kiddo in the picture to the right. If you can’t do it as well as that infant, then you are predisposed to injury. It’s as simple as that. We must squat, lunge, walk, climb stairs, push, pull, reach, etc. with proper mechanics, not because we are attempting to be elite level athletes, but simply because we are human beings and we must successfully build a solid movement foundation before we can build the walls of strength, flexibility, etc. around it.
“Success is doing the ordinary things extraordinarily well.”
– Jim Rohn
Not sure if you move correctly or not, schedule an evaluation with me and we will perform the Functional Movement Screen, a reliable and valid tool, to determine what weak links you may have that could eventually be the crack in your foundation, and then provide you with the proper tools to fix it before it becomes a bigger problem.

